Anyone can get an infection, but as with certain people in the community, many people in hospital environments have a higher risk of getting an infection because of chronic illness, age, or other risk factors. Hospitals and other healthcare facilities add extra risks:
Concentrated exposure to germs:
Healthcare facilities have other sick people who could spread infections. Patients see more people while they’re in a healthcare facility than they might normally (workers, volunteers, and visitors, for example). These people could unknowingly transfer germs from patient to patient.
Invasive interventions and devices:
Interventions that cause a break in your skin
or introduce a piece of medical equipment inside your body can cause an infection. The most common interventions that can cause an infection include:
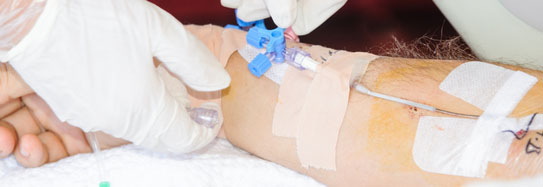
– Central lines (also called central venous catheters) – People who are seriously ill may have a central line, a special type of intravenous (IV) catheter. This allows nurses to effectively provide antibiotics or other medications and fluids.
A doctor inserts the central line into a large vein in your groin, chest or neck. Because these special IVs are in a large vein, they can stay in place for several weeks or longer. This eliminates the need to keep restarting IVs in the more delicate veins in the arm. However, a drawback is that these larger veins give more direct access to the heart, and infections can become very serious very fast.
A central line infection is a central line-associated bloodstream infection, or CLABSI.
More infections:
– Urinary tract infections – Patients in the hospital and in long-term care facilities may have a urinary catheter – a tube inserted into the urethra, which drains urine fr om the bladder. Infections resulting from a urinary catheter are catheter-associated UTIs, or CAUTIs. According to statistics, 75% of all UTIs in the hospital are CAUTIs, and they are the most common type of healthcare-acquired infection today.
om the bladder. Infections resulting from a urinary catheter are catheter-associated UTIs, or CAUTIs. According to statistics, 75% of all UTIs in the hospital are CAUTIs, and they are the most common type of healthcare-acquired infection today.
– Surgical site infection – If you have surgery, your wound is at risk for getting infected. The severity of the infection can range from a superficial infection in the skin around the surgical incision, to a much deeper internal infection. Surgical site infections are SSIs.
– Ventilator-associated pneumonia – When people are on a ventilator because they need help breathing, they are at risk for developing pneumonia, an infection in the lungs. Called ventilator-associated pneumonia, or VAP, there are many possible causes for this type of infection. They include exposing the lungs (from the tube) to bacteria that may not normally be able to reach the lungs.
– Pressure injuries – Patients how are confined to bed or spend extended time in a chair or wheelchair are at risk for developing a pressure injury or sore. Seniors can also have fragile skin that tears easily. These injuries can become infected, as well.


 om the bladder. Infections resulting from a urinary catheter are catheter-associated UTIs, or CAUTIs. According to statistics, 75% of all UTIs in the hospital are CAUTIs, and they are the most common type of healthcare-acquired infection today.
om the bladder. Infections resulting from a urinary catheter are catheter-associated UTIs, or CAUTIs. According to statistics, 75% of all UTIs in the hospital are CAUTIs, and they are the most common type of healthcare-acquired infection today.