Sepsis is a medical emergency. It needs to be treated as such. In other words, sepsis should be treated as quickly and efficiently as possible as soon as it has been identified. Treatment includes rapid administration of antibiotics and fluids. The risk of death from sepsis increases by an average of up to 7.6% with every hour that passes before treatment begins. (Critical Care Medicine)
Patients with severe sepsis or septic shock who are treated in an intensive care unit (ICU) can experience issues related to the illness and medications, the lack of sleep, and the overstimulation of having people and noise around them 24 hours a day. This can result in agitation, confusion, even hallucinations.
Treatment
(Looking for information about the treatment bundle used in most hospitals, known as SEP-1? Click here.)
Antibiotics
Physicians prescribe antibiotics (usually more than one type) based on the type of infection. Broad-spectrum antibiotics are the first-line medications. These antibiotics work against several of the more common bacteria. These are intravenous antibiotics so they can get into the blood system quickly and efficiently.
IV Fluids
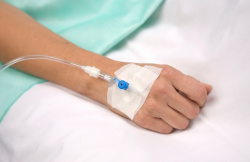
Antibiotics alone won’t treat sepsis; you also need fluids. The body needs extra fluids to help keep the blood pressure from dropping dangerously low, causing shock. Giving IV fluids allows the health care staff to track the amount of fluid and to control the type of fluid.
Ensuring the body has enough fluids helps the organs to function and may reduce damage from sepsis.
Several types of fluid
While there are several types of IV fluids, some are standard in treating sepsis. Normal saline is one commonly given fluid. It is a crystalloid fluid. These are fluids that contain minerals, such as sodium, and are water-soluble, or dissolve in water. These add fluid to the blood system.
Colloids, another type of fluid, are thicker fluids. For example, blood is a colloid. Colloids given by IV include albumin and dextran. Colloids do not dissolve as quickly as crystalloids. More crystalloid fluid is needed than colloid fluid to achieve the same goal of boosting body fluid volume, but crystalloids are less expensive.
Additional Possible Treatments and Equipment
Since all patients are different and there are many causes of sepsis, not every available treatment is right for each patient. To find out what treatment is being you or your loved one need and why, speak with your health care provider.
Here are treatments, medications, and types of equipment that may be used on a patient with sepsis or septic shock.
Extracorporeal Therapies
Extracorporeal therapies are treatments done using machines and techniques such as continuous renal replacement therapy (a type of dialysis) or extracorporeal membrane oxygenation, or ECMO (life support).
Special types of IVs
Arterial lines – Arterial lines look like IV lines but they go directly into an artery, usually the wrist or groin. Nurses can monitor blood pressure and take frequent blood samples without inserting a needle in a vein each time one is needed. A special cap protects the line. It allows blood draws directly from the line. The line and cap must be monitored closely because the pressure caused by the blood pumping from the heart can result serious bleeding if the line becomes undone.
Central lines – Central lines are large IV catheters most often inserted into a large vein near the shoulder. They they can go in any large vein, such as the neck or groin. Central lines have larger catheters than IVs. They provide fluids more quickly and easily. They also don’t need to be changed as often as an IV, which may be more comfortable for the patient.
Medications
Corticosteroids – Although doctors don’t know why corticosteroids work for some patients who have sepsis and not others, they can be helpful. Corticosteroids can help reduce inflammation in the body and depress the immune system, making it less active.
Vasopressors – Physicians prescribe vasopressors to patients who are in shock and whose blood pressures have dropped dangerously low. The vasopressors act constrict or tighten up the blood vessels, forcing the blood pressure to go up.
Oxygen – Patients usually get oxygen, by mechanical ventilator, mask or nasal cannula. This ensures the body has enough oxygen in its system. A pulse oximetry monitor, often called a pulse ox, is a small piece of equipment that fits over the tip of a finger or toe, or on the ear lobe. It measures the amount of oxygen in the blood.
Equipment
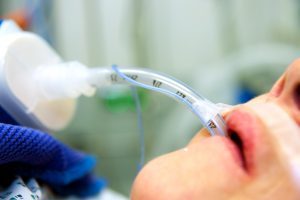
Endotracheal Tube – An endotracheal tube, or ET tube, goes through the mouth into the trachea (windpipe) and is attached to a ventilator. A patient who has an ET tube is intubated. When the tube comes out, they are extubated. Patients with ET tubes cannot speak as the tube passes through the vocal cords. If there is damage in the mouth but a patient needs intubation, the doctor can insert a nasotracheal tube through the nose. Patients who are intubated may be restrained, their hands fastened down, if there is a danger of them unknowingly pulling the tube out. The physicians may opt to perform a tracheostomy if a patient must be on a ventilator for an extended time or there is too much damage to the mouth or throat. The doctor makes an opening in the throat for direct access to the trachea. A tube is inserted through the opening, fastened down, and connected to the ventilator.
Intracranial Pressure Monitor – An intracranial pressure (ICP) monitor measures the fluid pressure in the brain. A sensor placed directly below the skull is attached to the monitor.
Kidney dialysis (renal replacement therapy) – Patients may need dialysis if their kidneys cannot filter the blood as they should. A portable dialysis machine allows patients to undergo dialysis in the ICU. A special catheter is inserted into a large vein and attached to the dialysis machine. Blood flows through the machine, which filters out toxins in the blood. This is what the kidneys normally do. Once the blood is filtered, it flows back into the body.
Mechanical ventilation – Ventilators, sometimes called respirators, help patients breathe. The machines can either do all the work for the patient by pushing the air into the lungs at a preprogrammed speed, or they may only help when needed. The machine records how often the patient breathes. If there are not enough breaths within a certain period, the machine will assist by taking over as needed.
Nasogastric Tube – A nasogastric (NG) tube goes through the nose and down into the stomach. When inserted through the mouth, it is called an oral-gastric tube, but through the nose is the most common approach. This tube may be connected to a suction bottle, which draws out stomach contents to help reduce nausea and vomiting.
PreSep™ catheter – This type of catheter monitors the oxygen levels in the blood that is returning to the heart.
Pulmonary artery catheter – This type of catheter goes into the pulmonary artery – the blood vessel that carries blood from the heart to the lungs, where the blood can be supplied with oxygen. “Pulmonary” means something is related to the lungs.
Urinary Catheter – A urinary catheter is a tube inserted through the urethra to the bladder. It helps drain urine into a bag attached to the side of the bed or strapped to a leg. Patients may need a urinary catheter for a few hours or indefinitely, depending on the situation. If the catheter remains in for an extended period, it needs to be changed according to the facility’s protocol.
Sepsis Alliance Connect is a virtual support community designed for the millions of people affected by sepsis. Click here to learn more or to sign up.
Updated March 25, 2021





























