WHAT IS ANTIMICROBIAL RESISTANCE?
What if water could no longer put out fire? What if, over time, fire evolved to outsmart water—raging uncontrolled to destroy everything in its path?
Now, imagine instead of fire, it’s germs. Specific strains of bacteria, viruses, fungi, or parasites that make people sick have adapted in order to avoid the antimicrobials (medicines such as antibiotics, antivirals, antifungals, and antiparasitics) designed to treat them. This is called antimicrobial resistance (AMR). These drug-resistant germs, also known as superbugs, are currently putting millions of people at risk of developing a life-threatening, untreatable infection.
ANTIMICROBIAL RESISTANCE: AN INVISIBLE ENEMY
While superbugs may sound like science fiction, they are a very real danger and can spread between people, animals, and the environment (through drinking water and soil).

ANTIMICROBIAL RESISTANCE: AN UNKNOWN ENEMY
In 2021, an online survey was carried out among 6,330 adults living in the United States, Brazil, China, India, and Spain. Globally, only half of adults surveyed (52%) were aware of the term antimicrobial resistance, but fewer had knowledge of the effects of AMR. Learn more about the survey conducted and the findings below.
KNOW YOUR RISK
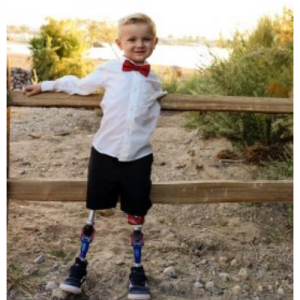
Who is at risk of infection with a superbug? In short: everyone. But AMR is hardest on people most vulnerable to infection:
- Young children and people over the age of 60
- People with underlying conditions like heart disease, chronic obstructive pulmonary disease (COPD), stroke, Alzheimer’s disease, diabetes, kidney disease, cancer, and people with autoimmune conditions.
SEPSIS AND ANTIMICROBIAL RESISTANCE (AMR)
Sepsis, which was often called blood poisoning, is the body’s overwhelming and life-threatening response to an infection and is one of the most significant health complications that can result from antimicrobial resistance. Like strokes or heart attacks, sepsis is a medical emergency that requires rapid diagnosis and treatment. Sepsis can lead to tissue damage, organ failure, and death.
How is an antimicrobial-resistant infection connected to sepsis? Antimicrobial resistance challenges the treatment of sepsis. As more germs become resistant to antimicrobial medicines used to treat infection, more people are at risk for developing sepsis.
A MAJOR PUBLIC HEALTH CRISIS
How did this happen? The answer is complicated, but two contributing factors are:
- Not taking antimicrobials as intended: taking them too often, unnecessarily, or not finishing a course of medicine. The more a germ is exposed to the same antimicrobials designed to take it down, the more likely it is to learn how to outsmart the medicine and survive.
- While superbugs have evolved, our antimicrobials have not. First widely used in the 1940s, antimicrobials (starting with the antibiotic penicillin) have saved millions of lives. But after this major discovery, there have been few new advancements.
Antimicrobial resistance means common medical procedures—dentist visits,
cesarean sections (C-sections), hip replacements, chemotherapy, and organ
transplants—will carry a greater risk of infection.
HOW CAN WE HELP TAKE DOWN ANTIMICROBIAL RESISTANCE?
Taking simple precautions can help us fight back. Remember: the POWER to defeat superbugs is up to us. Infection prevention is AMR prevention(tm).

Learn more about some superbugs that are currently in the news by clicking here.