Jenny Lorraine
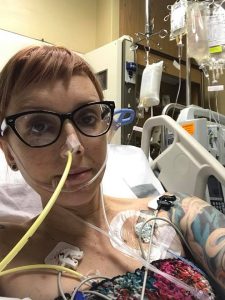
I’m not sure if my story is different than anyone else’s, but I will share it nonetheless. I’ve had sepsis three times and septic shock with liver failure once, all in a year and a half. I honestly don’t know how I survived any of it.
The first time I heard the S word, I was eight months pregnant with my third child, December 2015. (Sepsis and Pregnancy & Childbirth)
I had severe hyperemisis gravidarum, a deadly form of morning sickness. I had IVs 24/7, that ran medications, fluids, electrolytes, and calories. I felt a bit off all day, and my PICC line that fed me liquid nutrition (TPN) looked irritated. I had a temp of 99*F, and drove myself to the ER. (Sepsis and Invasive Devices)
Huge chunks of time are missing. It was the first time I saw those strange containers for blood cultures. The next thing I know, I’m laying in a bed, calling my husband Mike, at work. “I have sepsis. I’m so scared. Please hurry.” He was pulled over for speeding, and the officer let him go.
The rest of the hospital stay is blank. It doesn’t exist in my memory. I don’t know how long I was admitted, and I only know it was around Christmas, because of photos. My two oldest children spent Christmas morning at Denny’s with my mom.
I was released at some point, and back all too soon, because our son, Sullivan, was born two weeks later. He was perfectly healthy, and we went home to recover and start our new lives together. Soon, I fell into a severe postpartum depression, that teetered on psychosis. Looking back, I didn’t want to admit I was sick, or needed help. I even went back to work, and pretended life was normal.
It was far from that.
After my first sepsis baby was born, my husband and I thought it was all a fluke. The hyperemesis, the sepsis, the countless hospital stays – it was so awful, and we wanted a blissful pickles and ice cream pregnancy.
So we tried for one more baby. I found a doctor who specialized in hyperemesis gravidarum, and we created a plan, if I were to be sick again. We had no idea what we were getting into. Genetic testing, D&C, medication and four miscarriages later, I found myself pregnant again, and back at my OB’s office, getting a sonogram. Two babies! There was only one heartbeat, but it was strong. I miscarried the twin, and another horrific hyperemesis pregnancy began.
Sometime in April 2017, was the second time I had sepsis. I was about 14 weeks pregnant, and had a PICC line for fluids and medication. I felt sort of tingly and warm, took my temperature, and went to the emergency department. The insertion site of my PICC line looked slightly red and irritated, and a nurse pulled the line while I was in the ER. Cultures were taken, and I was admitted.
Again, my stay at the hospital is blank in my memory. Doctors tried another PICC insertion, but could not find suitable veins. Next step, a Groshong line. A Groshong is a heavy duty central line in one’s chest, and much like a PICC, it is able to deliver medications and fluids, but can stay longer in the body and has a lower risk of infection.
The cultures came back for the second bout of sepsis, and was a rare yeast the infectious disease doctor had never seen in 40 years of practice. Doctors actually used Google to find out more! (Sepsis and Fungal Infections)
The third time I had sepsis was a strange one. I sat on the couch on Mother’s Day 2017, and felt water on my shirt. My Groshong line had a tiny crack in it, and so back to the ER I went. Radiology was called to repair the line, a simple ten minute procedure.
When a dressing change is done on a PICC or central line, it is a sterile procedure, including the masks and gloves. I noticed one of the nurses put on gloves, left the room, and returned wearing the same gloves. Two nurses and one radiology doctor repaired the line without masks and sterile gloves. I lad on the table, petrified to speak up.
Two days later, I was in an ambulance and back in the hospital with sepsis. I was never angry with the non-sterile environment and risk they took with my health. I was angry at myself for not speaking up.
I had my Groshong line in for just over a month, when I became septic for the third time. I have really no memory of the hospital stay, nor how long it was, as sepsis has destroyed my memory. I do know I had the infected Groshong line pulled and a new one surgically placed. I went through all of these procedures alone.
I spent most of my hospital stays alone.
I was sent home, and placed on TPN, as I was getting zero calories and gained zero weight at 20 weeks of pregnancy. With TPN, a person should have regular blood draws to check their electrolyte panel. I never had a blood draw. A new home health care company took over my care, once I had TPN. I saw three different nurses in a week, and they all said different things.
The home health care company was incredibly unorganized. One evening, a bit too late for my taste, a random nurse came out to my home to do a dressing change. She had Mike, my husband, watch, and told me I can do my own dressing changes from now on.
That was the worst piece of advice I’ve ever heard.
About a week later, I called home health for a dressing change, as I am not going to change it myself in the mirror. I brought up the nurse who asked I change the dressings myself and the company was outraged. Not as much as I was, as they were charging my insurance company $35k a month for my care.
I asked for a different nurse to come out and care for my Groshong. The company tried to find one, and no one was available. Day after day, I called and begged for someone to come out, and was told no one was available. I began to get scared that an infection might begin. Three days after my dressing needed to be changed, another random nurse came to my home.
I was in bed, as I didn’t feel well. I felt weak, my dressing was hanging off, even though I taped it back, and there was a weird discharge coming from my line. I had TPN running 24/7, along with medications. Ten days with the same dressing, and I began to feel a sense of doom.
The nurse took my temp, and it was 99F, she changed my dressing and was heading out. I asked her to check my temperature one more time, and it was 104F. She said, “If you start feeling bad, call a doctor.”
And she left.
Moments later, I was violently vomiting, shaking, and turning a pale gray color. I was freezing cold. My teenager sat on my bed with me and urged me to call someone. I called a friend and no answer. The teenager begged me to call an ambulance, and the next thing I knew, I’m being wheeled out of the house, and telling my children I loved them.
I began hallucinating in the ambulance. (Sepsis and Hallucinations) One of the EMTs kept me as coherent as possible, as we discussed Gulf Coast seafood and our favorite restaurants. And then it goes blank.
I wake in the ICU, very confused.
I was hooked up to everything, two vasopressors, antibiotics, TPN, fluids, ventilator, and I don’t know what else. I was in sever septic shock and my liver was failing. I had a Dobhoff feeding tube placed.
There’s a photographic moment, clear as day, in my memory. An obstetrician, an RN, an anesthesiologist, and one more, I don’t recall. I had a couple bands around my waist to measure the baby’s heartbeat. I was 25 weeks pregnant.
It was surreal to hear a heartbeat go from the 160s, and just drop. The obstetrician placed her hand on my leg. The anesthesiologist asked if we could do a cesarean immediately. The obstetrician said there was no way I would make it through, and she said she was making the decision to save me, because I had children at home.
I said I have to deliver a dead baby?
She said I’m sorry.
I said when?
She said you have to get better and out of ICU. We can’t deliver now.
I said so I have to keep a dead baby inside of me?
She said I’m so sorry. I’m so sorry.
Everyone stood around me in silence, as I tried to process that my daughter died.
I said please call my husband.
They said to come quick. He did. A doctor spoke to him, outside of the room, told him the baby didn’t make it, and it’s not looking good for his wife, either.
There’s another block of time missing, but I glanced at my husband, his face in disbelief, no words, just confusion of what was happening.
I shopped for bassinets in the morning and cremation services in the evening.
Time passed. Minutes. Hours. Days. I felt something. A kick? My body betrayed me. And another? A soft movement, but I was drugged and delirious. My ICU nurse came in and I mentioned it, and she replied with remorse that it was my mind playing tricks. I asked her to please bring an OB and a sonogram, just to rest my mind.
Warm jelly and the ultrasound wand was now on my tiny 26-week belly, as I was still losing weight and did not look pregnant. The on-call OB scanned and had wide eyes. She saw a heartbeat, slow and floppy, but it was there. She couldn’t believe it, brought others into the room. Baby came back to life.
Everyone was in disbelief, including Mike and me. We were warned to expect a very disabled child, extreme disabilities, and possibly not surviving long.
Eventually, I was moved to the med/surg floor for recovery. Doctors tried several times to place feeding tubes, as I would vomit them up, was unable to speak, and one I yanked out in my sleep. I had seven placed during my fourth bout with sepsis.
The hospital stay is such a blur, and the days and nights run together. One morning, my obstetrician stopped in to say hello. He had a bewildered look on his face and bluntly said, “You should be dead.” I chuckled and replied, “You can’t get rid of me that easy!”
Baby was evaluated, had a good heartbeat, but still an unknown of what she would be like when born. So, we began a very difficult wait. I eventually was discharged from the hospital, and went home. I was incredibly weak, and needed a lot of help, but was too stubborn to ask. Looking back, I’m not sure how I dealt with day to day activities.
A few weeks later, I went into early labor and Juniper was born that evening via cesarean section. She weighed five pounds, and went to the NICU. I began my recovery from surgery and a hellish pregnancy.
When I was in ICU with septic shock, a blood clot formed. No one was aware of this, as I had no symptoms. I was so medicated and on pain killers, so I wouldn’t have noticed anything. Unbeknownst to me, this clot travelled to my heart and began to damage it. Eventually, it would move to my lung.
After Baby June was born, I’d visit her in the NICU every day. Recovering from two bouts of sepsis and one time septic shock, and a cesarean section, I was very weak and tired, but I never missed a day to visit.
About two weeks after she was born, I was drinking some beer in my bedroom, chatting with my family. I had this awful pain in my right ribs, but figured I pulled a muscle. I tried to ignore the pain, and had a fair share of Lone Star beer. The next day, the pain was still there, so I went to get it checked out at the hospital, after i was done visiting Baby June in the NICU. She came first, even though I was in pain. In the ER, x-rays and CT scans, and blood work was done.
The doctor came back, sat down, and put her hand on my hand. She said I had a massive pulmonary embolism and my right lung had died (she called it infarction). There was fluid surrounding my lung now, my heart had been damaged, and she said she couldn’t believe I was alive, with the extensive damage.
She asked what I had done the evening before, and I told her I had some beers and bitched about the pain to my husband and teenager.
The doctor chuckled.
She said that if I hadn’t been drinking, the pulmonary embolism would have absolutely killed me. Lone Star beer thinned my blood just enough for me to survive a massive blood clot killing my right lung. My heart and lung will never be the same, and I’ll be on lifelong medication, but thanks to Lone Star beer, I’m alive.
I never thought I would have a PE! I didn’t know anything about them. I feverishly googled while in the ER, and while I was admitted. The doctor asked what I wanted to do, and gave me a couple options to try and deal with this pulmonary embolism. I remember saying, “Let’s get this party started!” and was immediately admitted and started medication.
I had two surgeries to drain fluid around the lung. Two bouts of pneumonia following, which was more hospital stays, one of those, having an anaphylactic reaction to medication I was given. It is surreal how many times I’ve come close to death.
A year later, I open my eyes each morning and reach for pain killers. Three out of the seven I take each morning. My joints and back are in excruciating pain. My muscles, weak. My brain suffered similar to a stroke, and is not the same. My lung, still scarred and will never be the same, and still hurts with a deep breath or yawn. My heart, permanently damaged, as well.
Simple things like walking or breathing are so painful. Picking up a baby makes me grit my teeth in pain. Day in and day out, I grin and bear it. Sometimes, I use a cane just to get around. I don’t feel like I’m living. I’m just barely surviving.
I have nightmares several times a week. Flashbacks. Anxiety and fear of becoming sick. I don’t like to leave the house, because there are germs outside. Post septic syndrome comes with a laundry list of debilitating symptoms. (Sepsis and Post-Sepsis Syndrome)
I have a pulmonologist, hematologist, cardiologist, EP cardiologist, pain clinic, and gastroenterologist. I wear two medic alert bracelets. Seven medications a day, that’s an improvement from the fourteen I was taking less than a year ago. I have a handicap placard for the car.
Coming that close to death didn’t give me a new lease on life. It’s left me alive, but broken. It doesn’t seem like a celebration. It’s more of mourning who I used to be.
2020 UPDATE:
It’s been two and a half years since I last had septic shock. My dreams and everyday life blend together, and memories do not form right. The effects from Post-Sepsis Syndrome are still very strong, and continue to affect my everyday life. Sepsis caused a pulmonary embolism, which still causes issues like pain and breathing problems, and I am in the hospital for pleurisy every few months.
Sepsis damaged my heart so badly that I finally had surgery in November 2019, which didn’t quite go as planned, and a month later, I found myself having surgery again for a pacemaker. I never imagined I would be just 40 years old, and have a pacemaker. No one warns you what sepsis or septic shock can leave you with. Or should I say take away?
The daily pain, braces, cane, and meds have become just part of me. Don’t get me wrong, I’m thankful and astounded I’m here, but there’s a great deal of survivor’s guilt, as well as anger and sadness that this is my life now.
https://www.facebook.com/jennylorrainesepsis/


























