Harold McDuffie II

On Saturday September 17, 2011, I woke up feeling very winded and short of breath. Taking just 3 steps felt like running 3 miles. The day before I had to cut my daily 2-mile walk short because I just didn’t feel “right.” When my wife came home she thought I should go to the local town hospital and I was in no condition to argue.
When the staff took my blood/oxygen level, it was at 40% and the x-rays showed my lungs partially filled with fluid. They gave me oxygen and tried to make me as comfortable as possible. At this point I probably figured I just caught a bout of pneumonia and would get some antibiotics and go home. I couldn’t have been more wrong. The doctor said I needed to be transported to the intensive care unit in Little Rock, an hour away. When I got there they ran more tests and told me I would have a lung biopsy on Monday and would need to go on a ventilator. The results from the weekend tests and biopsy confirmed a sepsis infection. My lungs were bleeding and almost completely filled with fluid at this point.
In addition to the sepsis, I had gone into acute respiratory distress syndrome (ARDS), and my kidneys had started to fail. Even with being given 100% oxygen, my blood oxygen was still very low. The docs told my wife that I had a less than 35% chance of surviving this and to prepare for the worst, but because of my relatively young age and being in good condition, I had a better chance than most at coming through. (Sepsis and ARDS)
Over the next 4 weeks, I was placed in an induced coma, had a tracheotomy, was given a feeding tube, and had all kinds of IVs, wires an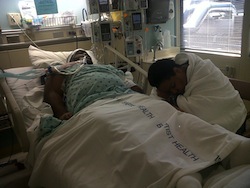 d hoses coming out of me. My fever was over 103.5 for almost a week as the staff worked tirelessly to keep me cool, including cooling blankets and ice. At this point my lungs were completely filled and not working at all on their own. I was totally dependent on the ventilator for survival. After the 4th week and several surgeries to drain fluid from my lungs and antibiotics to combat the sepsis, I finally began to turn the corner.
d hoses coming out of me. My fever was over 103.5 for almost a week as the staff worked tirelessly to keep me cool, including cooling blankets and ice. At this point my lungs were completely filled and not working at all on their own. I was totally dependent on the ventilator for survival. After the 4th week and several surgeries to drain fluid from my lungs and antibiotics to combat the sepsis, I finally began to turn the corner.
Slowly I became less dependent on the ventilator and needed less oxygen. By October 17, I had been moved to recovery and gradually regained full lung and kidney function. The nurses who had been working on me from day one called me a living miracle, as they didn’t think I was going to make it. As I continued to recover and heal, I was told that I could not go home right away and would have wait until I was strong enough to go to physical therapy and learn how to walk again as my leg muscles had atrophied as a result of the intubation and bed rest.
After 11 more days of grueling therapy, on November 2, I was able to walk out of the hospital with a walker and finally go home to my wife and my 3 children, who couldn’t understand why daddy went away for so long. As for the cause of what brought on the sepsis, the docs were at loss, and then my wife remembered that for the previous two months, I had been taking a high dose (100mg) of prednisone, a steroid, for a chronic eye infection and that it probably weakened my immune system and left me defenseless against even a common cold.
To this day I am left with very painful peripheral neuropathy in my legs and have to use a cane to get around, but I am alive and give all thanks and praise to God that he saved me not only from sepsis, but also ARDS and gave me a second chance at life. (Sepsis and Post-Sepsis Syndrome)































