The Connection Between COVID-19, Sepsis, and Sepsis Survivors
March 19, 2020
If you know someone who has died from an infection, such as pneumonia or a urinary tract infection, you know someone who has died from sepsis. Sepsis is your body’s toxic reaction to an infection. As your body’s immune system tries to fight the infection, it may go into overdrive and start attacking the body itself instead. Any infection, including viral infections like the flu and COVID-19, caused by the novel coronavirus, can cause sepsis. This can lead to serious illness, even death.
COVID-19 and sepsis
Last week, the medical journal The Lancet, published a study that reviewed case histories of 191 people in China hospitalized with COVID-19, 54 of whom died. The researchers found that patients who were severely ill or had died:
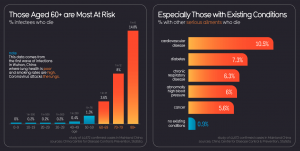
- Were older and/or
- Had sepsis and/or
- Had problems with blood clotting
Given that death from infection is due to sepsis, these findings are not surprising. But perhaps they can help physicians determine treatment plans for their more severely ill COVID-19 patients. They do know how to treat sepsis: IV fluids, appropriate antimicrobials when needed, and supportive care depending on which organs are affected.
Other research has shown that pre-existing conditions, such as heart disease and diabetes also increase your risks related to COVID-19.
Seeking help
Unfortunately, the first signs of COVID-19, or symptoms from a mild version, can be similar to sepsis signs and symptoms. People who have fever, cough, and shortness of breath should call their doctor or contact their local COVID-19 information/advice line if there is one available before to going to see a doctor or nurse practitioner in person. Patients can also check if their doctor’s office or clinic offers telemedicine services. Many have started offering this service. This outreach can provide patients with initial screening, helping them decide if they should be seen in person or can stay home and monitor their health.
People with early stages of an infectious illness, either this coronavirus or any other disease, should avoid emergency room or urgent care waiting rooms. If they have the virus, they could spread the disease to others in the waiting room. If they don’t have the virus, they themselves may be exposed to it by someone else in the waiting room. This is why the guidance from Centers of Disease Control and Prevention (CDC) is for patients to remain at home but to seek care if they are developing signs of respiratory distress (difficulty breathing, shortness of breath).
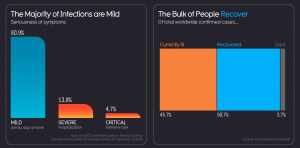
Fevers caused by COVID-19 can last for days. And about 80% to 85% of patients have mild symptoms. If someone has more severe symptoms such as intensifying shortness of breath, this would be a concern for sepsis. Other signs of sepsis such as a change in mental status (confusion, excessive sleepiness); a drop in urine output; or worsening fever, pain, or overall illness, would also be an emergency.
Sepsis survivors and COVID-19
Since COVID-19 is a viral infection, it puts you at risk of developing sepsis. But people who survived sepsis or septic shock are concerned they may be at higher risk of contracting the infection. It is true that people who survive sepsis and septic shock are more vulnerable to getting other infections, any type of infection. This higher risk results from weakening of the immune system in the first few weeks and months following the initial bout of sepsis. It is for this reason that social distancing and self-isolation is even more important during this pandemic.
How social distancing and self-isolating works
There have been memes on social media that show how social distancing and isolation can help stop infection spread, but a clip from the comedy Scrubs (2006), shows how germs spread, no matter how unintentionally. Follow the germs, in glowing green:
Majority of COVID-19 infections are mild
It is true that most people who develop COVID-19 recover after experiencing only mild symptoms. So, why is everyone so concerned?
It goes back to no one knows who will develop complications like sepsis and that the landscape keeps changing. We know that sepsis survivors and those who have chronic illnesses or weakened immune systems, as well as the elderly are at higher risk. But there have been increasing numbers of younger previously healthy individuals who have become so seriously ill that they had to be hospitalized, some needing ventilators and life support. Their mortality, or death, rate might not be as high as people at high risk, but they could need long, intense, and expensive care to recover. If they have sepsis, their journey may not end when they get home, since many sepsis survivors are left with long-lasting effects, such as post-sepsis syndrome, post-traumatic stress disorder, and more.
To learn more about sepsis and associated infections, visit our Sepsis and… library.





























