Group B Strep, A Danger to Infants: GBS Awareness Month
July 6, 2018
When a baby is born, parents worry about several things, but one thing many may not know about is the potential risk of infection from group B streptococcus (GBS). According to the Centers of Disease Control and Prevention (CDC), about 25% of pregnant women, 1 in 4, carry the bacteria, but most aren’t aware. It is possible to have the bacteria in your gastrointestinal tract or genital tract, but not have any symptoms of infection. And if it’s undetected, you can pass GBS to your baby during childbirth, putting him or her at risk for sepsis.
While not all babies who are exposed to GBS get sick, 1.7 babies out of every 1,000 live births who are exposed do develop an infection, and GBS infection is the leading cause of early-onset sepsis among infants. Early-onset sepsis is sepsis that occurs within the first 7 days of life. Late-onset sepsis can occur up to 3 months of age.
Preventing GBS infection in infants
Since it’s known that one-quarter of pregnant women carry GBS, screening programs and treatment with antibiotics during labor and delivery can significantly lower the number of babies who are infected. Screening for GBS is non-invasive and painless. Your doctor, nurse, or midwife uses a swab to collect a sample from your vagina when you are between 35 to 37 weeks pregnant. This sample is then tested for the bacteria. Testing earlier in the pregnancy may give a negative finding (no bacteria), but this doesn’t guarantee that GBS may not be pregnant closer to delivery, which is why earlier testing is not recommended.
If the sample shows you are carrying GBS, you should receive antibiotics while you’re in labor and throughout delivery to reduce the risk of you passing on the bacteria. Babies whose mothers have GBS infection but who don’t get IV antibiotics during labor and delivery have a 1 in 200 chance of being born with GBS disease. Babies whose mothers have GBS and do receive treatment have only a 1 in 4,000 chance of having GBS disease.
If you have not tested positive with the swab test but you have had a positive urine test for GBS any time in your pregnancy or you have had a previous baby who developed GBS disease, you should automatically be given antibiotics during labor and delivery and do not need to have the screening test.
Why treatment during labor only?
Group B strep grows very quickly. If you take antibiotics before you go into labor, the bacteria can grow back and still infect your baby. Antibiotics, most often penicillin, by intravenous (IV) while you are in labor is the best protection for your baby. If you are allergic to penicillin, other antibiotics can be used, but penicillin is the first choice to treat GBS.
If you fall into one of the categories where you should be treated for GBS and if you go into labor early, it is vital that you tell the doctors and nurses about your GBS status, particularly if you in a facility where you are not known. They can prepare the proper IV treatment to help keep your baby safe from infection.
Babies exposed to GBS
Group B strep in newborns most often causes pneumonia, meningitis, and sepsis. The most common symptoms in babies are:
- Fever
- Difficulty feeding
- Irritability or lethargy
- Difficulty breathing
- A bluish tint to the skin
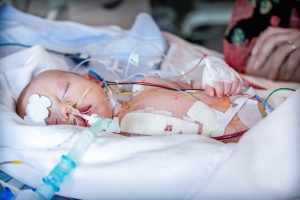
GBS in babies is treated with antibiotics, most often penicillin or ampicillin. However, if your baby becomes seriously ill, more advanced treatment may be necessary and your baby may be moved to the neonatal intensive care unit (NICU) for specialized care.
Group B strep in older children and adults
Information about GBS tends to focus on babies because this is the age group most commonly affected by the bacteria, but GBS can also infect older children and adults. The symptoms you would develop as an adult would depend on what part of the body is infected by GBS. For example, if you have pneumonia, you might find experience breathlessness, coughing, fever, and chest pain. But if you have an infected cut, you may have increased redness and pain around the cut, pus, and a fever.
Some people are at higher risk of contracting a GBS infection than others. This includes those who are older than 65 years, or who have chronic illnesses, like diabetes and heart disease.
To learn more about GBS and how it relates to sepsis, please visit Sepsis and Group B Streptococcus, part of the Sepsis Alliance Sepsis and… series.





























