Losing Limbs to Sepsis: Limb Loss Awareness Month
April 1, 2019
One of the most life-altering complications that affects thousands of sepsis survivors is amputation of one or more limbs. Statistics show that there are over 1.6 million amputations in the United States every year; 10% of these are due to complications from sepsis. People who go into septic shock may develop small blood clots in their blood vessels, which prevent adequate blood flow to their fingers, hands, arms, toes, feet, and legs. The blood carries vital oxygen and nutrients and if the body’s tissues are deprived of these, they begin to die. April is Limb Loss Awareness Month, dedicated to raising awareness of this issue that too many sepsis survivors have experienced.
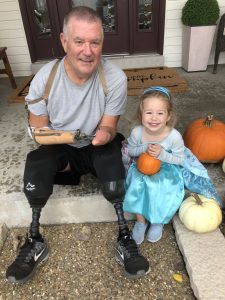 Rusty Wagstaff, a 58-year-old sepsis survivor in Wendell, N.C., knows about amputations. Five years ago, Rusty developed sepsis, possibly from a group A streptococcus infection and pneumonia. After the initial urgent treatment to save his life, he had to undergo amputations of all four limbs: his left hand, his right arm below the elbow, and both legs below the knee. “It’s no doubt this journey is a life-changing event,” Rusty says. “But death would have been much worse.”
Rusty Wagstaff, a 58-year-old sepsis survivor in Wendell, N.C., knows about amputations. Five years ago, Rusty developed sepsis, possibly from a group A streptococcus infection and pneumonia. After the initial urgent treatment to save his life, he had to undergo amputations of all four limbs: his left hand, his right arm below the elbow, and both legs below the knee. “It’s no doubt this journey is a life-changing event,” Rusty says. “But death would have been much worse.”
When a limb is damaged because of tissue death, amputations are the last resort. If you develop gangrene, your surgeon may first try to remove just the dead tissue (debriding) if it’s not covering too large an area. The hope is the blood flow to the still healthy tissue will be strong enough to keep the area well nourished. Another treatment for gangrene is hyperbaric oxygen therapy. Patients spend time in an environment that delivers oxygen at high levels and the extra oxygen may encourage healing. But if debriding and other treatments like hyperbaric oxygen therapy aren’t options or they don’t work, amputation is the next step.
How amputations are decided
If there are multiple amputations, they may be done in stages. Rusty became ill a week before Christmas and was the sickest on Christmas Day, he says. “They amputated my legs on January 2nd.They amputated my hands on the 15th.”
When planning surgery, orthopedic surgeons study the limb or limbs to try to remove as little as possible, minimizing later disability. Some people may have only toes or fingers amputated, while others may have part or most of their leg or arm removed. Sometimes surgeons plan on one approach, such as a below-the-knee amputation, but once the surgery starts, they may see that there is too much damage and need to amputate above the knee instead.
Life after amputations
Surviving sepsis can leave many challenges. Some people complain that they never felt right again once they went home, living with chronic pain, fatigue, post-traumatic stress disorder (PTSD), and more. But if amputations are also part of their survival, this may result in drastic changes to the most basic tasks and lifestyle. But it is possible. “Almost everything you do going forward will take longer than it used to,” Rusty says. “Be patient! Everything comes with a new challenge.”
Rusty suggests that people with limb loss try to find something to do outside that they enjoy. “You will learn to appreciate life in a different way,” he explains. Your amputations may also make you a center of attention, something you might not be used to. But this isn’t necessarily a bad thing, Rusty believes. “Get used to people (especially children) staring. They will want to ask questions and I love sharing. They will want to help you do things. Let them because it makes them feel good.”
There’s no doubt that limb amputations change your life. They require lifestyle changes for you and the ones you love, particularly when you are first learning how to use prosthetics or a wheelchair. But there are groups and organizations that may help you. If you are struggling, speak with your doctor, physical therapist, or occupational therapist about where you can get help.
The risk of amputations may be lowered if sepsis is recognized and treated as quickly as possible, before it begins to cause damage to your body. If you have any reason to suspect that you or someone you know has sepsis, call 911 and tell the operator that you suspect sepsis. Think TIME™:
- T- temperature, which may be higher or lower than normal
- I- infection. There may be signs or a procedure that may have caused an infection.
- M- mental status. The patient becomes drowsy, confused, or difficult to rouse.
- E- extremely ill, “I feel like I might die.”
It may not only save a life, it may save limbs.



























